Medical Student Education
Highlights
- The University of Wisconsin School of Medicine and Public Health (UW SMPH) launched “Human Family Tree,” the fourth course in its new ForWard curriculum. Gregory Rice, MD, was the course’s integrated block leader, and Allison Pollock, MD, and Ashley Kuhl, CGC, were assistant integrated block leaders.
- Department faculty continued to play key roles in the design and implementation of the ForWard curriculum, as follows:
Curriculum Transformation Steering Committee
- Anna Huttenlocher, MD
- Gwen McIntosh, MD, MPH
- Elizabeth Petty, MD
Longitudinal Teacher/Coaches
- Eileen Cowan, MD
- Troy Kleist, MD
- Kathleen DeSantes, MD
- Amy Plumb, MD
Phase 1: Human Family Tree
- Gregory Rice, MD
- Ashley Kuhl, CGC
- Allison Pollock, MD
Phase 2: Care Across the Life Cycle
- Eileen Cowan, MD
- Kirstin Nackers, MD (integrated block leader and department block leader)
- Casey Reiser, MS, CGC
Phase 3 Activities
Matthew Harer, MD, (pediatrics portion of internship prep course design leader) with Melissa Cercone, MD, Mary Ehlenbach, MD, Sushant Srinivasan, MD, and many Pediatrics fellows, residents and collaborators.
Residency
Highlights
- University of Wisconsin Department of Pediatrics faculty, residents and staff partnered with the Midwest Consortium of Global Child Health Educators to pilot a “boot camp” to prepare learners for the clinical, emotional and ethical challenges of a global health experience.
- Resident Derek Spindler, MD, attended the national conference of Solutions for Patient Safety (SPS), a network of children’s hospitals that aims to create universally safe healing environments. Building on the affiliation with SPS, he was the resident representative for a working group that developed Culture of Safety classes at American Family Children’s Hospital, which have since been rolled out hospital-wide. He was also the resident representative on an American Family Children’s Hospital task force to improve the process by which stat medications are ordered and delivered in the Pediatric Intensive Care Unit, and participated in a project to reduce the risk of tissue damage due to calcium chloride extravasation.
Dr. Spindler and resident Alison Taber, MD, were also members of the UW Health Resident Quality and Safety Council, a multi-specialty working group that reviews and reports on patient safety issues, participates in root cause analysis sessions, and brainstorms ways for quality improvement.
- Residency faculty presented research at the spring meetings of the Pediatric Academic Society and the Association of Pediatric Program Directors showing that peer assessment of residents at our institution highly correlated with faculty assessment of residents, particularly among senior residents assessing interns and with respect to professionalism. These results demonstrate that peer assessments are a valid tool for our clinical competency committee (CCC) to use when assessing residents’ sub-competency milestones.
In addition, the CCC incorporated comments from patients at residency continuity clinics, and from nurses who directly observe residents on the wards, into resident performance assessments. The committee synthesizes this feedback, along with statements on current progress and future directions, and provides it to residents twice a year to integrate into their individualized learning plans.
- Resident Matthew Rysavy, MD, received the department’s 2017 resident research award for his analysis of ways to improve reporting of extremely preterm birth outcomes, and was the lead author in the resulting article published in the September 2016 issue of Pediatrics. In 2017, he was a co-author on a New England Journal of Medicine article on survival and neurodevelopmental outcomes of infants born at the borderline of viability.
- In an effort to expand educational opportunities for learners, the department matched its first joint Pediatrics-Neurology resident, Hui “Katie” Li, MD, PhD, in 2017. Dr. Li earned her MD and PhD in neurology at China’s Tongji Medical College of Huazhong University of Science & Technology. In academic year 2017-2018, she’ll begin the first of two years in the UW Department of Pediatrics before completing the shared residency in the UW Department of Neurology.
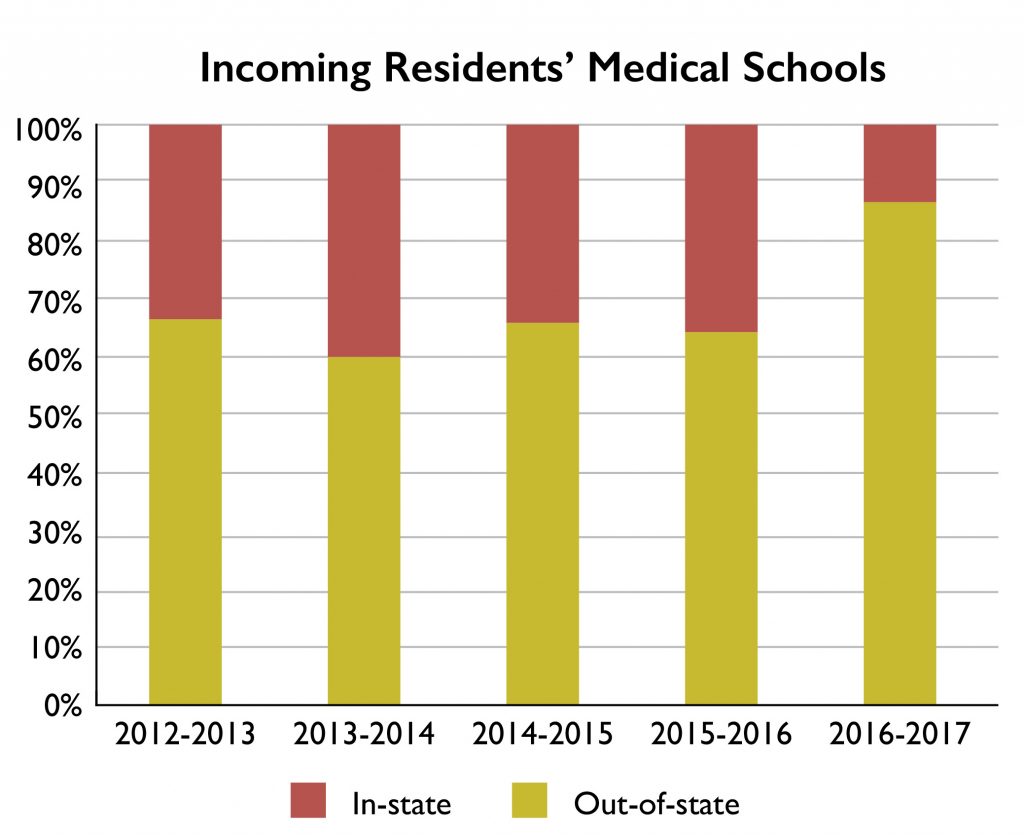
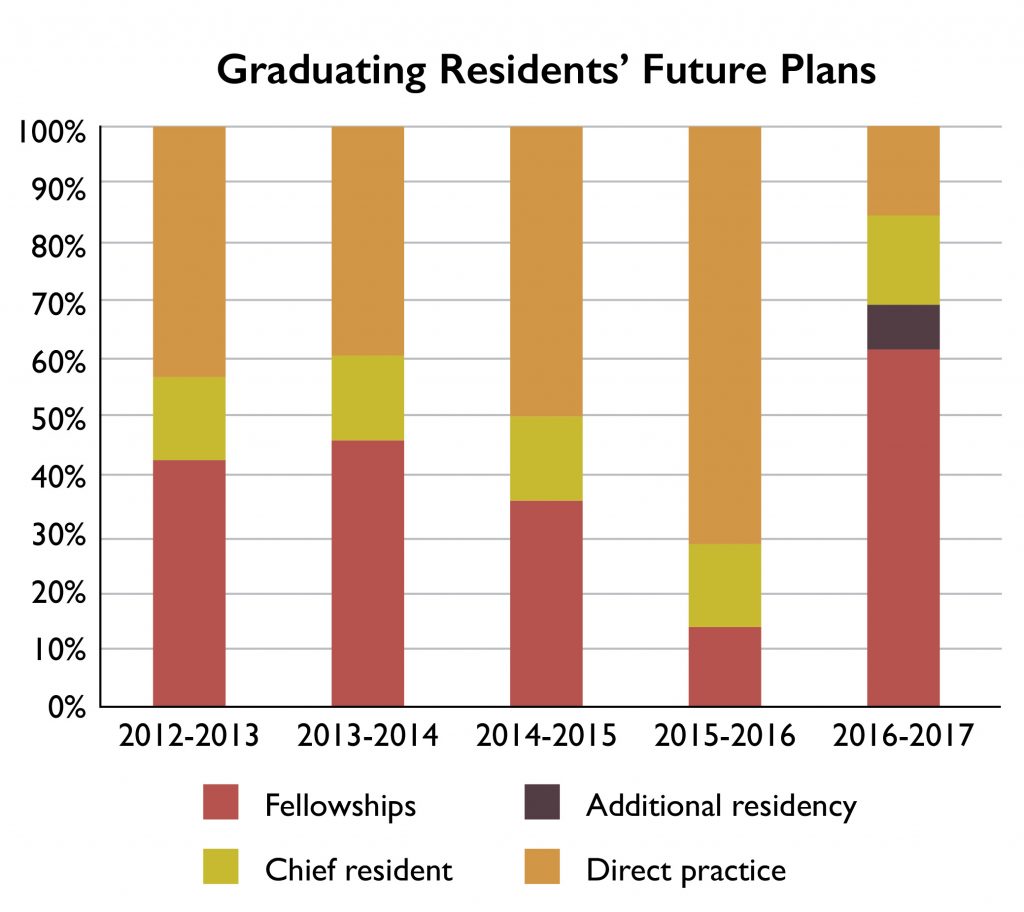
2016-2017 Residents
 |
 |
 |
 |
|
Nicole Bentley, MD Medical School |
Ashley Carver, MD Medical School |
Alissa Enzenberger, MD Medical School |
Alexandra Erdmann, MD Medical School
|
 |
 |
 |
 |
|
Jennie Godwin, DO Medical School |
Alexander Golec, MD Medical School |
Daniel Gorski, MD Medical School |
Dane Hammer, MD Medical School |
 |
 |
 |
 |
|
Hou-Xuan Huang, MD Medical School |
Santhi Logel, MD Medical School |
Kristen Marten, DO Medical School |
Katherine Omernick, MD Medical School |
 |
 |
 |
|
|
Anisha Rimal, MD Medical School |
Michael Smith, MD Medical School |
Helen Waterman, DO Medical School |
 |
 |
 |
 |
|
Christina Amend, MD Medical School |
Jeff Clark, MD Medical School |
Thomas L. Devries, MD Medical School |
Alexis J. Gumm, MD Medical School |
 |
 |
 |
 |
|
Erick Jimenez, MD Medical School |
Nicole N. Kamps, MD Medical School |
Perry J. Krumenacher, MD Medical School |
Ashley Przybilla, MD Medical School |
 |
 |
 |
 |
|
Matthew A. Rysavy, MD, PhD Medical School |
Kathryn M. Schmit, MD Medical School |
David Shafique, MD Medical School |
Sadie J. Skarloken, MD Medical School |
 |
 |
 |
|
|
William Stanford, MD Medical School |
Jennifer E. Szmanda, DO Medical School |
Diana Vu, MD Medical School |
 |
 |
 |
 |
|
Amanda Becker, MD Postgraduate Plans |
Michael Fenster, MD Postgraduate Plans |
Daniele Gusland, MD Postgraduate Plans |
Tyce Kearl, MD, PhD Postgraduate Plans |
 |
 |
 |
 |
|
Allison Lindell, MD Postgraduate Plans |
Mitchell Luangrath, MD Postgraduate Plans |
Kathleen Miller, MD Postgraduate Plans |
Rachel Petro, MD Postgraduate Plans |
 |
 |
 |
 |
|
Nicholas Pytel, DO Postgraduate Plans |
Derek Spindler, MD Postgraduate Plans |
Shannon Summers, MD Postgraduate Plans |
Allison Taber, MD Postgraduate Plans |
 |
|||
|
Mariam Wahidi, MD Postgraduate Plans |
Fellowships
In academic year 2016-2017, we had 29 fellows in nine programs.
Highlights
- Allergy and immunology fellow Halie Anderson, MD, (mentor: Daniel Jackson, MD) received the Asthma Diagnosis & Treatment Interest Section Fellow-in-Training Outstanding Abstract Award at the 2017 American Academy of Allergy Asthma and Immunology (AAAAI) annual meeting. Her abstract, “Increased rhinovirus-induced innate immune response in peripheral blood during infancy is associated with improved lung function at school age,” was also selected for the meeting’s featured poster session.
- Hematology, oncology and bone marrow transplant fellow Miriam Kim, DO, received a two-year St. Baldrick’s Fellowship Award that, with her mentor Christian Capitini, MD, will support her project, “Developing MSC-derived exosomes to enhance HSCT for pediatric leukemia.”
- Infectious diseases fellow Emma Mohr, MD, PhD, received the 2017-2019 Pediatric Infectious Diseases Society’s Stanley and Susan Plotkin and Sanofi Pasteur Fellowship Award for her project, “Development of a Macaque Congenital Zika Syndrome Model: Fetal Zika Virus Tissue Distribution and Pathology.” Dr. Mohr was also a co-author on PLoS Pathogens articles on maternal-fetal Zika virus transmission in pregnant rhesus macaques and the mechanisms of Pegivirus in a macaque model of HIV infection.
Infectious diseases fellow Joseph McBride, MD, was a co-author with Dr. Klein on a Clinical Chest Medicine article reviewing the clinical manifestations and treatment of blastomycosis.
2016-2017 Fellows
 |
 |
 |
 |
|
Claudette Adegboro, MD Subspecialty Prior Residency |
Daniel Adu, MD Subspecialty Prior Residency |
Evelyn Angulo, MD Subspecialty Prior Residency |
Tarun Malkani, MD Subspecialty Prior Residency |
 |
 |
 |
 |
|
Yashoda Naik, MD Subspecialty Prior Residency |
Lucianne Olewinski, MD Subspecialty Prior Residency Postgraduate Plans |
Sima Ramratnam, MD Subspecialty Prior Residency |
Cheryl Steiman, MD Subspecialty Prior Residency |
 |
|||
|
Julie Voeller, MD Subspecialty Prior Residency |
 |
 |
 |
 |
|
Halie Anderson, MD Subspecialty Prior Residency Postgraduate Plans |
Christina Barreda, MD Subspecialty Prior Residency |
Adam Bauer, MD Subspecialty Prior Residency |
Kelly Bush, MD Subspecialty Prior Residency |
 |
 |
 |
 |
|
Jamee Castillo, MD Subspecialty Prior Residency Postgraduate Plans |
Erin Hammer, MD Subspecialty Prior Residency |
Lauren Kanner, MD Subspecialty Prior Residency |
Miriam Kim, DO Subspecialty Prior Residency |
 |
 |
 |
 |
|
Angela Lager, PhD Subspecialty Doctoral Degree Postgraduate Plans |
Kristy Lee, PhD Subspecialty Doctoral Degree Postgraduate Plans |
Emma Mohr, MD, PhD Subspecialty Prior Residency |
Vu Trieu Nguyen, MD Subspecialty Prior Residency |
 |
 |
||
|
Imran Sayed, MD Subspecialty Prior Residency |
Subspecialty Prior Residency |
 |
 |
 |
 |
|
Maria (Cora) Astorga, MD Subspecialty Prior Residency Postgraduate Plans |
Christina Bryndzia, DO Subspecialty Prior Residency Postgraduate Plans |
Joseph McBride, MD Subspecialty Prior Residency Postgraduate Plans |
Robert Strait, MD Subspecialty Prior Residency Postgraduate Plans |
 |
 |
||
|
Adam Szadkowski, MD Subspecialty Prior Residency Postgraduate Plans |
Khoon Queenie Tan, MD, PhD Subspecialty Prior Residency Postgraduate Plans |
Continuing Professional Development (CPD)
Highlights
-
-
Approximately 130 primary care physicians, nurses, and physician assistants attended the 2017 Seminars in Pediatrics to learn about current trends in pediatric research and clinical practice. This year’s focus was on opioid and substance use disorders in children; Kristin Shadman, MD, and Mala Mathur, MD, MPH, served as course directors.
Keynote speaker Lucien Gonzalez, MD, MS, FAAP—a pediatric addiction medicine expert at the University of Minnesota—gave two talks on the rise of pediatric opioid and substance use, and how pediatricians can better understand, identify and help children and young adults with these disorders.
Two pre-conferences were also held prior to Seminars:
-
- “Adapted Motivational Interviewing Self-Assessment,” a facilitated American Board of Pediatrics Part 2 Activity; and
- “Getting Down and Dirty with Fracture Splinting.”
-
-
-
- UW Department of Pediatrics faculty, residents, fellows, and students came together to spotlight research accomplishments during the department’s 2017 Spring Research Day, held Friday, May 12, 2017, at the Health Sciences Learning Center. This year’s Research Day also included 71 abstracts by faculty, fellows and residents, a 20 percent increase from 2016. Of these, 25 (35%) were accepted at the Pediatric Academic Society meeting: 13 as poster presentations, 10 as platform presentations and two as workshops.
-
- Patricia Emmanuel, MD, chair of the Department of Pediatrics at the University of South Florida–Tampa, spoke at the department’s annual Gilbert Barness Lectureship. The title of her presentation was “The Pitfalls of Molecular Diagnosis in Infectious Diseases.”
-
- Several department faculty are testing a new American Board of Pediatrics (ABP) pilot to replace the traditional Cognitive Expertise — Secure Exam (Part 3). The ABP introduced a different method for assessing the knowledge of pediatricians as part of Maintenance of Certification (MOC). This pilot, called MOCA-Peds (Maintenance of Certification Assessment for Pediatrics) involves shorter, more frequent assessment of pediatricians’ knowledge and will include an additional learning component not typically found in other types of assessments.
-
- Maria A. Stanley, MD, FAAP, served as the committee co-chair for the 2017 Down Syndrome Medical Interest Group–USA (DSMIG-USA®) Annual Symposium. This national conference, held in Sacramento, California, brought together 115 attendees.
- Mollie Kane, MD, MPH, along with residency alumna Jessica McGee, MD, facilitated the Iams lectureship ABP MOC Part 2 Activity, “Adolescent Medicine.”