I feel that every baby everywhere deserves the best care to allow them to survive and thrive.
As a neonatologist and a painter, I promote Advocacy, Research, and Teaching as part of the ART of medicine. Inequities in healthcare have a negative impact on neonates and their families worldwide. I am committed to partnering with people in our community and globally to work on ways to eliminate healthcare inequities and improve neonatal care.


Professor
mcadams@pediatrics.wisc.edu
Advocacy for Neonatal Health and Equality
Injustice anywhere is a threat to justice everywhere.
Dr. Martin Luther King, Jr., Letter from Birmingham Jail
 |
 |
Racial inequities, both in the U.S. and globally, jeopardize the well-being of countless infants and children. Every child deserves clean air, safe water, sanitation, shelter, nutritious food, and access to high-quality healthcare. They have an inherent right to the best possible start in life.
In Wisconsin, we confront two alarming racial disparities: high infant mortality rates for Black babies and low exclusive breastfeeding rates. Addressing these challenges head-on, the Meriter Foundation generously supported our initiative: A Pregnancy, Birth, and Lactation Support Program to Boost Exclusive Breastfeeding Rates among African American Women.
Teaming up with the Tia Murray, Founder & CEO of the Harambee Village Doulas, and the African American Breastfeeding Alliance, our project centered on a comprehensive early pregnancy, birth, and lactation support strategy to elevate exclusive breastfeeding rates for Black infants. The Doula Model of Care—a cornerstone of our approach—prioritizes emotional and physical support, cultural respect, and evidence-based education to empower mothers during pregnancy, childbirth, and postpartum. The results were promising: approximately 96% of mothers breastfed at discharge, with roughly 79% exclusively breastfeeding.
Advocacy extends beyond our home. Most neonatal challenges occur in low-and-middle-income nations. Fueled by a passion to make a difference, I’ve volunteered in countries like Peru, Mongolia, Cambodia, Zambia, Malawi, Uganda, and India, focusing on elevating neonatal care in resource-limited settings. We must work towards a world where every infant, irrespective of race or region, gets an equal opportunity at a healthy life.
This is an accordion element with a series of buttons that open and close related content panels.
Publications and projects related to public and global health
Tomlin BD, McAdams RM, Zapata JY, Kaluarachchi DC. High Black infant mortality in Wisconsin: factors associated with the ongoing racial inequity. J Perinatol. 2021 Feb;41(2):212-219. doi: 10.1038/s41372-020-00906-6. Epub 2020 Dec 18. PMID: 33339984.
Delzer ME, Kkonde A, McAdams RM. Viewpoints of pregnant mothers and community health workers on antenatal care in Lweza village, Uganda. 2021. PLoS ONE 16(2): e0246926.
Garcia-Prats AJ, McAdams RM, Matshaba M, Thahane L, Butteris SM, Conway JH, Slutsker M, St Clair NE, Haq H. Mitigating the Impacts of COVID-19 on Global Child Health: a Call to Action. Curr Trop Med Rep. 2021 May 11:1-7.
Namiiro FB, Mugalu J, McAdams RM, Ndeezi G. Poor birth weight recovery among low birth weight/preterm infants following hospital discharge in Kampala, Uganda. BMC Pregnancy Childbirth 2012;12(1):1.
McAdams RM, Erdenebileg A, Batra M Zagd G. Health care provider attitudes toward non-initiation and withdrawal of neonatal resuscitation for preterm infants in Mongolia. Journal of Population, Health, and Nutrition 2012 Sep;30(3):346-52
McAdams RM, McPherson RJ, Batra M Zagd G. Antenatal parental counseling in Mongolia: a countrywide survey of Mongolian health care providers. Maternal and Child Health Journal. 2013 Jun 27
Hedstrom A, Ryman T, Otai C, Nyonyintono J, McAdams RM, Lester D, Batra M. Demographics, clinical characteristics and neonatal outcomes in a rural Ugandan NICU. BMC Pregnancy Childbirth. 2014 Sep 19;14:327
McAdams RM. Bubble CPAP may be safe and efficacious for neonates in low and middle income countries, but more evidence is needed. Evid Based Med. 2015 Feb 9. pii: ebmed-2014-110135
McAdams RM, Hedstrom AB, DiBlasi RM, Mant JE, Nyonyintono J, Otai CD, Lester DA, Batra M. Implementation of bubble CPAP in a rural Ugandan NICU. Respiratory Care. 2015 Mar;60(3):437-45
Delzer ME, Kkonde A, McAdams RM. Viewpoints of pregnant mothers and community health workers on antenatal care in Lweza village, Uganda. 2021. PLOS ONE 16(2): e0246926.
Mandepally A, Stanker C, Larson T, McAdams RM, Project Solar Filter, a device to help decrease disease from air pollution cause by particulate matter from biofuels. Rice 360° 11th Annual Global Health Technologies Design Competition, selection as a Semi-Finalist Team. March, 2021. https://www.youtube.com/watch?v=NU5h_hihrAs&t=6s
Art work related to Advocacy
- Original painting entitled “Transposition.” Academic Medicine 2010 Nov; 85(11): Cover Art. https://journals.lww.com/academicmedicine/Fulltext/2010/11000/Artist_s_Statement__Transposition.36.aspx
- Original painting entitled “Champei’s Petals.” Academic Medicine. 2012 Oct: 87 (10): Cover Art. https://journals.lww.com/academicmedicine/Fulltext/2012/10000/Artist_s_Statement___Champei_s_Petals.34.aspx
- Original painting and poem entitled “The Abruption.” Obstetrics & Gynecology. 2013 Dec: Cover Art (http://links.lww.com/AOG/A450). http://download.lww.com/wolterskluwer_vitalstream_com/PermaLink/AOG/A/AOG_122_6_2013_10_22_MCADAMS_000000_SDC1.pdf
- Original painting entitled “Wait and See.” Academic Medicine. 2014 Feb;89(2): Cover Art. https://journals.lww.com/academicmedicine/Fulltext/2014/02000/Artist_s_Statement___Wait_and_See.21.aspx
- Original painting entitled “The Orphans.” Academic Medicine. 2014 Sep;89(9): Cover Art. https://journals.lww.com/academicmedicine/Fulltext/2014/09000/Artist_s_Statement___The_Orphans.13.aspx
- Original painting entitled “The Girl in Blue.” Academic Medicine. 2016 May;91(5): Cover Art. https://journals.lww.com/academicmedicine/Pages/toc.aspx?year=2016&issue=05000
- Original painting entitled “In the Face of Hunger.” Academic Medicine. 2017 Aug;92(8): Cover Art. https://journals.lww.com/academicmedicine/toc/2017/08000
- Original painting entitled “The Absent Multitude.” Academic Medicine. 2018 Dec;93(12) Cover Art. https://journals.lww.com/academicmedicine/toc/2018/12000
- Original painting entitled “Lost Stars.” Academic Medicine. 2019 Dec 94(12). Cover Art. https://journals.lww.com/academicmedicine/toc/2019/12000
- McAdams RM. Beauty of Breastfeeding. Journal of Human Lactation. 2021;37(1):13-14. doi:10.1177/0890334420966973
Research
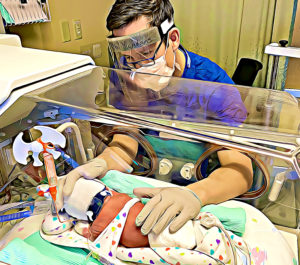
Perinatal brain injury can be devastating to babies and to their families. My hope is that through research, we can understand ways to prevent brain injury in babies and treat babies with brain injury to help optimize their neurodevelopmental outcomes.
Hypoxic ischemic encephalopathy research
 Hypoxic ischemic encephalopathy (HIE) results from reduced oxygen and blood flow to a fetus or newborn, leading to potential complications like brain damage. In the U.S., HIE affects about 1.5 in every 1000 live births.
Hypoxic ischemic encephalopathy (HIE) results from reduced oxygen and blood flow to a fetus or newborn, leading to potential complications like brain damage. In the U.S., HIE affects about 1.5 in every 1000 live births.
Using the secure, HIPAA-compliant database, Peri-Data.Net®, we identified several antenatal and intrapartum risk factors for HIE:
Antenatal Factors: First-time motherhood, History of fetal death/stillbirth, Antidepressant usage, Illicit drug use, Rh factor sensitization, and Excessive gestational weight gain
Intrapartum Factors: Placental abruption, Uterine rupture, Heavy meconium in amniotic fluid, and Cesarean-section deliveries
Notably, 70.3% of infants with HIE had at least one intrapartum risk, versus 29.6% without HIE. Our ongoing research is exploring how fetal heart rate patterns, combined with the above factors, can better predict HIE risks. The ultimate goal? Informing obstetrical decisions to reduce HIE occurrences.
This is an accordion element with a series of buttons that open and close related content panels.
Publications related to perinatal brain injury
McAdams RM and Juul SE. Cerebral Palsy: Prevalence, Predictability, and Parental Counseling. NeoReviews 2011;12; e564-e574
McAdams RM and Juul SE. The role of cytokines and inflammatory cells in perinatal brain injury. Neurology Research International 2012:561494
McAdams RM, McPherson RJ, Mayock DE, Juul SE. Outcomes of extremely low birth weight infants given early high-dose erythropoietin. Journal of Perinatology2013;33(3):226-30
Traudt CM, McPherson RJ, Bauer LA, Richards TL, Burbacher TM, McAdams RM, Juul SE. Concurrent erythropoietin and hypothermia treatment improve outcomes in a term nonhuman primate model of perinatal asphyxia. Developmental Neuroscience. 2013;35:491-503
McAdams RM, McPherson RJ, Kapur R, Phillips B, Shen DD, Juul SE. Dexmedetomidine reduces cranial temperature in hypothermic neonatal rats. Pediatric Research 2015;77:772-778
McAdams RM, McPherson RJ, Beyer RP, Bammler TK, Farin FM, Juul SE. Dose-dependent effects of morphine exposure on mRNA and microRNA (miR) expression in hippocampus of stressed neonatal mice. PLoS ONE. 2015 Apr 6;10(4):e0123047
McAdams RM and Juul SE. Neonatal encephalopathy: Update on therapeutic hypothermia and other novel therapeutics. Clinics in Perinatology. 2016 Sep;43(3):485-500.
McAdams RM, McPherson RJ, Kapur RP, Juul SE. Focal Brain Injury Associated with a Model of Severe Hypoxic-Ischemic Encephalopathy in Nonhuman Primates. Developmental Neuroscience. 2017;39(1-4):107-123
McAdams RM, Fleiss B, Traudt C, Schwendimann L, Snyder JM, Haynes RL, Natarajan N, Gressens P, Juul SE. Long-Term Neuropathological Changes Associated with Cerebral Palsy in a Nonhuman Primate Model of Hypoxic-Ischemic Encephalopathy. Developmental Neuroscience 2017;39(1-4):124-140
McAdams RM. Increased Odds of Survival or Prevention of Severe Neurological Injury in Extremely Low-Gestational-Age Neonates: Including Placental Transfusion as the First Step to Improve Outcomes in Preterm Newborns. JAMA Netw Open. 2019 Mar 1;2(3):e191293.
Peebles PJ, Duello TM, Eickhoff JC, McAdams RM. Antenatal and intrapartum risk factors for neonatal hypoxic ischemic encephalopathy. J Perinatol. 2020 Jan 40: 63–69
McAdams RM, Pak D, Lalovic B, Phillips B, Shen DD. Dexmedetomidine Pharmacokinetics in Neonates with Hypoxic-Ischemic Encephalopathy Receiving Hypothermia. Anesthesiol Res Pract. 2020 Feb 25;2020:2582965.
Berube MW, Puia-Dumitrescu M, McAdams RM. Does mild hypoxic ischemic encephalopathy adversely affect neurodevelopmental outcome? Journal of Perinatology.2021 Mar 13. doi: 10.1038/s41372-021-01026-5. PMID: 33714978.
McAdams RM, Berube MW. Emerging therapies and management for neonatal encephalopathy-controversies and current approaches. Journal of Perinatology. 2021 Mar 12. doi: 10.1038/s41372-021-01022-9. Epub ahead of print. PMID: 33712717.
Collaborators:
Dr. Claudette Onyelobi Adegboro, Neonatology
Theresa M. Duello, PhD. Director Diversity Initiatives, Associate Professor, Department of Obstetrics and Gynecology
Artificial Intelligence (AI) in Neonatal Care
In the NICU, we deal with a vast and often overwhelming amount of data. The health and well-being of critically ill infants hinge on the accuracy and timeliness of our decisions. Despite the sea of information available to us, traditional decision-making methods sometimes fall short, leading to preventable medical errors.
To advance neonatal care, we need to find the best ways to integrate AI into our approach. AI isn’t just about computers; it’s about enhancing the way we think, reason, and continuously improve. Here’s why AI is transforming neonatal health care:
- Advanced Learning: AI grows and adapts using progressive learning algorithms. It learns from patterns and improves over time.
- Deep Data Analysis: With its capability to delve deep into complex data, AI offers insights that might be missed with traditional methods.
- Reliability: AI can handle high-volume tasks efficiently, consistently, and without fatigue, ensuring that every data point is considered.
- Machine Learning in Neonatal Care: A pivotal part of AI, machine learning, focuses on using data and iterative processes to learn specific tasks without explicit programming.
We are at the forefront of this exciting intersection of neonatology and AI, striving to provide the best care for every infant.
 As a member of Neonatal Machine Learning and Innovations, Development, and Artificial Intelligence (NeoMIND-AI), we seek to to leverage the power of artificial intelligence (AI) to enhance the quality and precision of clinical care for neonates, in order to create a future where neonatal care is more personalized, efficient, and effective, and where every child has the best possible start in life.
As a member of Neonatal Machine Learning and Innovations, Development, and Artificial Intelligence (NeoMIND-AI), we seek to to leverage the power of artificial intelligence (AI) to enhance the quality and precision of clinical care for neonates, in order to create a future where neonatal care is more personalized, efficient, and effective, and where every child has the best possible start in life.
This is an accordion element with a series of buttons that open and close related content panels.
Publications related to A.I.
McAdams RM, Kaur R, Sun Y, Bindra H, Cho SJ, Singh H. Predicting clinical outcomes using artificial intelligence and machine learning in neonatal intensive care units: a systematic review. Journal of Perinatology 2022 May 13.
Singh H, Kusuda S, McAdams RM, Gupta S, Kalra J, Kaur R, Das R, Anand S, Kumar Pandey A, Cho SJ, Saluja S, Boutilier JJ, Saria S, Palma J, Kaur A, Yadav G, Sun Y. Machine Learning-Based Automatic Classification of Video Recorded Neonatal Manipulations and Associated Physiological Parameters: A Feasibility Study. Children (Basel). 2020 Dec 22;8(1):E1. doi: 10.3390/children8010001.
Singh H, Cho SJ, Gupta S, Kaur R, Sunidhi S, Saluja S, Pandey AK, Bennett MV, Lee HC, Das R, Palma J, McAdams RM, Kaur A, Yadav G, Sun Y. Designing a bed-side system for predicting length of stay in a neonatal intensive care unit. Scientific Reports. 2021 Feb 8;11(1):3342. doi: 10.1038/s41598-021-82957-z.
Sun Y, Kaur R, Gupta S, Paul R, Das R, Cho SJ, Anand S, Boutilier JJ, Saria S, Palma J, Saluja S, McAdams RM, Kaur A, Yadav G, Singh H. Development and validation of high definition phenotype-based mortality prediction in critical care units. JAMIA Open. 2021 Mar 25;4(1):ooab004. doi: 10.1093/jamiaopen/ooab004.
Teaching and Training
Virtual Reality in Neonatal Education
In today’s fast-evolving medical landscape, we recognize the need to transcend traditional boundaries in neonatal education. Virtual Reality (VR) is enabling us to achieve just that, adding depth, realism, and interactivity to the learning process.
Here’s what makes our VR-driven approach stand out:
- Immersive Learning Environments: With VR, learners don’t just observe—they experience. Using both avatar and video-based representations, participants can dive into 3D virtual environments that replicate real-life hospital settings.
- Global Collaboration: This technology breaks geographical barriers. It allows for real-time collaboration with experts from around the world, broadening horizons and sharing diverse expertise.
- Safe & Repetitive Training: Practice makes perfect. In our virtual hospitals, learners can safely repeat scenarios, ensuring they’re equipped to handle real-world challenges.
- Dynamic Participation: Rather than passive observation, VR encourages active involvement. This ensures a deeper understanding and retention of the material.
- Reflective Feedback: After the virtual sessions, learners can revisit their experiences. This introspection, combined with expert feedback, paves the way for continuous improvement.
Our journey in VR-based neonatal education has been enriched through partnerships. In collaboration with Dr. Sarah Trinh, a Neonatal-Perinatal Medicine fellow, we’ve spearheaded VR simulation projects both in Madison and Vietnam. Join us as we redefine the frontiers of neonatal education and training.
Redefining Neonatal Education and Training: Neonatal VR Simulation with Acadicus

Our OWLS Neonatal Simulation Team uses new technology & evidenced-based medical knowledge to train neonatal providers how to best care for babies. https://twitter.com/WiscPedsOWLS



