Congenital heart disease can be detected either prenatally by ultrasound or after birth by physical examination. Despite continuing advances in prenatal care, normal prenatal ultrasounds will fail to detect significant congenital heart disease in many babies. Fetal echocardiography can be performed if a problem is suspected on the routine ultrasound. Although fetal echocardiography is an excellent tool for evaluating an unborn baby’s heart, it is labor intensive and not widely available.
Physical examination is an invaluable part of the care of the newborn baby, but has some important limitations. Even when some forms of critical congenital heart disease are present, there may be no outward signs of a heart problem such as a heart murmur, breathing difficulties, decreased pulses, or abnormal skin color.
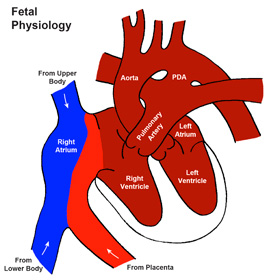 In order to understand how this could happen, it helps to know a little about how a baby’s heart works before birth. Before birth, oxygen is provided from the placenta and not from the lungs. It is not efficient to send all the blood to the lungs and the fetal circulation is designed so that blood is diverted away from the lungs. There is a large connection between the artery to the lungs (pulmonary artery) and the artery to the body (aorta) called the ductus arteriosus. Before birth, these three blood vessels are of similar size. While in a baby is in the womb, the ductus arteriosus connects the blood flow to the lungs and the body and may serve as a detour around problems within the heart.
In order to understand how this could happen, it helps to know a little about how a baby’s heart works before birth. Before birth, oxygen is provided from the placenta and not from the lungs. It is not efficient to send all the blood to the lungs and the fetal circulation is designed so that blood is diverted away from the lungs. There is a large connection between the artery to the lungs (pulmonary artery) and the artery to the body (aorta) called the ductus arteriosus. Before birth, these three blood vessels are of similar size. While in a baby is in the womb, the ductus arteriosus connects the blood flow to the lungs and the body and may serve as a detour around problems within the heart.
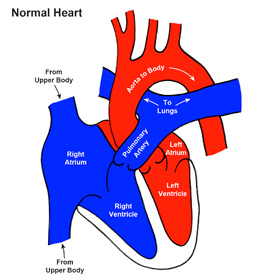
Before birth, however, the right heart (right atrium and right ventricle) and the left heart (left atrium and left ventricle) work together to take blood from the body and placenta and pump it back to the body and placenta. After birth, the right atrium and right ventricle (right heart) take blood from the body and pump it to the lungs and the left atrium and left ventricle (left heart) take blood from the lungs and deliver it to the body.
The ductus arteriosus remains open for the first few days after a baby is born and usually closes after the baby has gone home from the hospital. When still open after birth, it is referred to as a patent ductus arteriosus or PDA. In a child with critical congenital heart disease the PDA may still serve as an important detour and allow the heart and lungs to function quite well. However, as the PDA closes and the detour is lost, these children may become very ill very quickly.
 When someone examines a newborn baby, they will usually listen to the heart, check the pulses in the legs (femoral pulses), and look at the baby’s color. There is a significant blind spot in the physical examination as all three of these can be normal even in the presence of a critical heart defect.
When someone examines a newborn baby, they will usually listen to the heart, check the pulses in the legs (femoral pulses), and look at the baby’s color. There is a significant blind spot in the physical examination as all three of these can be normal even in the presence of a critical heart defect.
A heart murmur is a sound made by moving blood. Many factors determine the qualities of a heart murmur, but how much blood is moving and how fast it is going are the two most important. In some types of heart defects, little or no blood crosses one of the heart valves. Even though that heart valve function is very abnormal, there may be no associated heart murmur. Usually a heart murmur will eventually be present if there is a hole between the two pumping chambers (ventricular septal defect or VSD). However, this may not develop until the baby is a few days old, and may never be obvious in some of the most severe forms of congenital heart disease.
If the blood flow to the lower body is blocked by an important narrowing of the aorta, it may be difficult to feel the pulses in the legs (femoral pulses). However, if the PDA allows blood to be diverted around the narrowing, the baby’s femoral pulses will be normal.
The types of heart problem in which the PDA allows blood to be detoured around a blockage or narrowing are referred to as ductal dependent lesions. In these heart problems, the PDA allows one side of the heart to help out the other. If there is a blockage in the aorta, the right side of the heart can help out the left heart. If there is a blockage in the pulmonary artery, the left heart can help out the right heart. When one side of the heart is helping the other, there is a mixing of the low oxygen blood from the body and the high oxygen blood from the lungs. When this happens, the oxygen concentration in the baby’s blood will be abnormally low.
Unfortunately, our eyes are only able to detect severely decreased blood oxygen levels as a blue coloration of the skin called cyanosis. The amount of oxygen carried in the blood going to the body can be measured with a device called a pulse oximeter which tells what percentage of the blood’s potential to carry oxygen is being used. In a normal baby, the oxygen saturation will be greater than 95% by the time the baby is 24 hours old. Color changes in the skin due to low oxygen levels are reliably seen only when a baby’s oxygen saturation has dropped down into the 70% range. In many of the ductal dependent lesions, babies have oxygen saturations in the 80% range or higher. These saturations are clearly abnormal, but not visible to our eyes.
The failure of these three evaluations to detect ductal dependent heart disease can be thought of as a blind spot in the physical examination of the newborn baby.