It was a case of respiratory failure.
UW Health critical care transport team brought the patient to the American Family Children’s Hospital emergency department (ED). After stabilization, the patient was moved to the intensive care unit (ICU) for further care.
Physicians, nurses, residents, pharmacists, respiratory therapists and child-life specialists were called in throughout as needed. Afterwards, they debriefed on how the process could have been even safer and more effective.
The catch? The “patient” was a manikin, and the scenario was a simulation. But the clinician learning was very real.
Improving Interprofessional Team Function
The scenario was part of an interprofessional simulation project between the Department of Pediatrics, the BerbeeWalsh Department of Emergency Medicine and the UW Health Clinical Simulation Program.
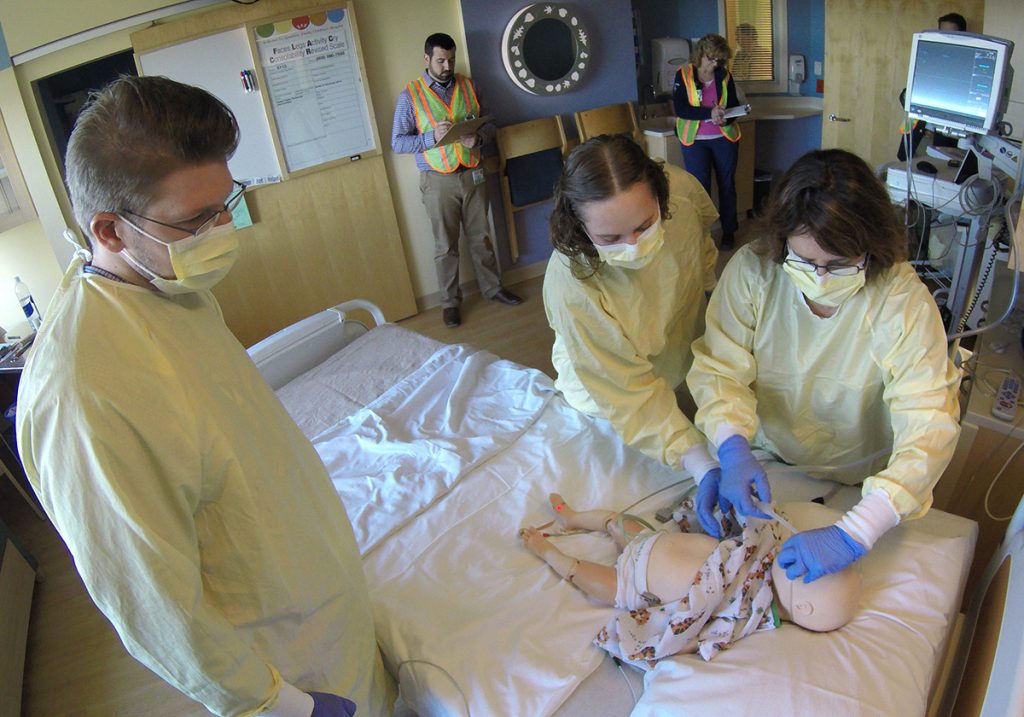
Last year, the team practiced the ED-to-ICU transport simulation multiple times. This year, they’re holding a series of simulations focused on rapid response for patients on the wards who need critical-care evaluation. All of the simulations replicate real-life situations and aim to improve transitions of care.
Melissa Cercone, MD, who now serves as the Department of Pediatrics’ director of simulation, said that the projects provide an opportunity to observe how an interprofessional team communicates and works together. For example, during a post-simulation debrief, an ED nurse can get a better understanding of what takes place in the ICU, and vice versa.
“It can open a lot of doors when it comes to effective function as a team,” Dr. Cercone explained. “A lot comes from a shared appreciation of others’ perspectives.”
After a simulation, the team debriefs and each participant has an opportunity to share observations, which can then be used to further improve care.
This model of simulation and debrief can be used in a variety of clinical environments to identify latent hazards, test new or existing systems and facilitate improvements. In January, Dr. Cercone and colleagues gave a workshop on it at the 2017 International Meeting on Simulation in Healthcare.
Building on Simulation in Residency, Outreach Programs
Simulation has been a key part of the department’s residency and outreach programs for several years.
Pediatrics residents strengthen procedural and communication skills through weekly sessions at the Clinical Simulation Program. Simulation is also woven into the interactive case-based discussions at Friday PEARL conferences.
Sushant Srinivasan, MD, leads the department’s Pediatric Advanced Life Support+ (PALS+), which attracts practicing clinicians from around the region.
He, along with Scott Hagen and Joshua Ross, MD, have also conducted emergency response simulations—using low-fidelity manikins—at several UW Health pediatric clinics.
Strengthening Clinical, Medical Student Education
Dr. Cercone hopes to continue these types of interprofessional and simulation activities at AFCH in the future.
Dr. Srinivasan is also working with the Clinical Simulation Program to develop a simulation instructor training program. The goal is that such a program can optimize the growth of simulation in the School of Medicine and Public Health’s new internship prep course for fourth-year medical students.
“There is a real art to conducting an effective debrief so learners achieve the objective you had intended,” Dr. Cercone noted. “The way to effectively use simulation is to think carefully about what are you looking to get out of it, because then you ask the right questions.”